WHY CAN’T MY BABY BREASTFEED?
Congratulations! You have just given birth to a gorgeous new baby. There are a few more joyous moments in life. You likely spent the last nine months entirely focused on your pregnancy and the new life you created – you dreamed of meeting your baby and the love it would bring to your life. You were glowing! As a new Mother, this is (supposed to be) the absolute most blissful time in your life.

You may have had a rude awakening that new parenthood is not what you expected. After three months of morning sickness, (likely) 6 more months of sore joints and fatigue, not to mention the weight gain AND then (in the best of outcomes) a very challenging delivery; now you have a HUGE and immediate job of feeding your child. Right when your body needs to rest and recuperate from the amazing physical triathlon your body just endured, AND your hormones are wreaking even more havoc on your body, you now must buck up and run even faster with very little sleep. Your blissful bubble just popped.
In the best-case scenario, all of the necessary details of biology generally work for you and your baby and establish breastfeeding with little trouble.
It will usually take a week or two to establish a good milk supply, “break-in” your nipples so they can endure your baby’s strong suck without pain or damage, and find comfortable nursing positions for you both.
You may have learned breastfeeding is more complex than you ever expected. Often, getting the help of a professional Lactation Consultant with milk supply issues or positioning is all that it takes to iron out the kinks.
Sometimes that’s just not the problem.
When breastfeeding challenges occur, the problem is often not with the mother’s technique but with the baby himself- barriers within the alignment and tone of his body causing abnormal function and preventing normal breastfeeding.
Let’s break this down.
What needs to happen for breastfeeding to be successful?
Your baby has to have a normal latch.

Your baby must be able to open their mouth wide enough to get much of your areola into the mouth.
The milk ducts are deep within this breast tissue. If the baby has a shallow latch (and cannot open the mouth widely), they will be clamping down on your nipple. This clamping down not only hurts and can cause damage to your nipple, but it also doesn’t access the deep milk ducts – making milk transfer much harder. Your baby must work much harder than they should to feed and might tire quickly, fall asleep at the breast, and/or feed too often to feel full.
Why can’t my baby open their mouth normally?
A baby not being able to open their mouth the normal way is usually due to the misalignment of the jaw.
The TMJ or temporomandibular joint (the jaw) is the union of the temporal bone, which sits just lateral to the upper neck and the Mandible. Your baby’s cranium and spine are not fused and are very pliable. Issues of abnormal in-utero positioning and the birth process can cause these bones to shift out of normal alignment.
Your baby has to have the normal use of his tongue.
Your baby must be able to squeeze your breast tissue tightly to the roof of his mouth to create a vacuum seal and suction pressure to transfer milk. If your baby does not have normal use of their tongue, they likely can not drain the breast completely. You might become painfully engorged, leading to mastitis. You might also have a low milk supply as they cannot stimulate enough production. Stimulating enough production is a complicated topic. Some possible barriers can prevent normal tongue function:
- “Tethered Oral Tissues” – Tethered Oral Tissues occur for two different reasons (and sometimes both occur at the same time) – genetic tethered oral tissues and structural tethered oral tissues.
- Genetic tethered oral tissues – We often hear this called a tongue-tie or Ankyloglossia. True Ankyloglossia (Tongue-Tie) definition is a condition in which a short, thick, or tight band of tissue (lingual frenulum) tethers the bottom of the tongue’s tip to the floor of the mouth. These ties can also occur under the upper lip or between the cheek and gums. This tie is a “midline defect,” forming during embryonic development due to a genetic mutation of the gene MTHFR (Methylenetetrahydrofolate Reductase) that helps process folate. In the case of true genetic tethering, your baby may need to have a surgical release of these tissues – often performed by a pediatrician, an ENT doctor, or a specialized Pediatric dentist with scissors or a laser.
- Structural Tethered Oral Tissues – Six main muscles form the tongue and allow it to move in all the needed ranges of motion for feeding and speaking. These muscles originate and are attached to various cranial and spinal bones- mainly to the Temporals, the Mandible, and the Hyoid bone in the upper neck. If these bones are imbalanced (again – due to in-utero positioning and the pressures of birth), then these tongue muscles are tethered and tight. This scenario might be present combined with Ankyloglossia. In either case, taking your baby to a specially trained Pediatric Chiropractor to gently adjust the cranium and spine can be very helpful to restore normal function.
2. “Cranial Nerve Impairment” – All of the functions of our bodies (including muscle action) require at least one nerve to allow its movement. In the case of the tongue, the main nerve supply is Cranial Nerve XII, the Hypoglossal nerve. This nerve originates in the brainstem and then passes through a small opening (called the Hypoglossal Canal) located deep within the upper skull/neck junction. The HG Canal sits inside the Occiput (the bottom skull bone), just medial to the condyles that articulate with the first neck vertebra (the atlas). The nerve then travels through the upper cervical spine to the angle of the Mandible (lower jaw) and dives deep to the tongue. Misalignment of any of these boney structures causes it to be impaired, resulting in weak muscles of the tongue.
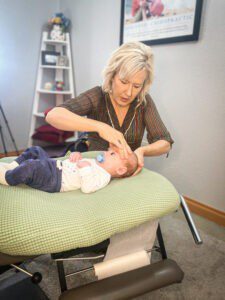
3. “Abnormal Palate Alignment” – As I mentioned earlier, your baby’s tongue must be able to press your breast tissue tightly to the roof of his mouth (the palate). Sometimes the palate can be abnormally high, making this job even harder. The palate forms in two ways:
- The Alignment of the Palate Itself – The hard anterior portion of the palate forms by the Maxilla. The Maxilla sits below the nose and connects to the jaw and the temporal bones on each side of the face (via the Zygomatic arch). The soft posterior portion of the palate makes the Palatine bone. The Palatine bone connects to the Maxilla (in the front) and the Sphenoid bone (in the back), which connects to the Temporal bones and the Occiput. Once again, alignment is the key to the proper function of this area.
- The Normal Use of the Tongue – Now this comes back full circle! The arch of the palate partially forms by the tongue pressing up against it during fetal development. If the tongue does not have a normal range of motion (for all of the reasons discussed above), there can be an abnormal palate development.
The take-home message of this article is to have hope.
If you and your baby struggle to breastfeed, there are usually apparent explanations when we look at the anatomy.
There are also straightforward, effective, and gentle ways to help.
- Seek out a certified and skilled Lactation Consultant to address aspects of feedings such as supply, breast health, and positioning.
- Seek out a certified and experienced Pediatric Chiropractor to address aspects of feeding such as the baby’s latch and tongue control.
- You might need to seek out a professional for an evaluation and release of genetic tethered oral tissues if they are present.
There is an abundance of good help available to you. There is a plethora of research to support the benefits of breastfeeding- physically, neurologically, and emotionally.
To learn more about breastfeeding and the anatomy involved in infants and how it affects breastfeeding, real-life case studies with breastfeeding patients, a host of interviews with lactation consultants, diagrams, demonstrations, and visual examples to teach the global subluxation pattern – The Anatomy of Breastfeeding. This new, updated, accredited continuing education course is for Chiropractors who are looking to improve their careers, learn from leaders and experts in their industry, and looking for new opportunities! The course is approved for 10 chiropractic CE hours.
“Breastfeeding is not just a method of delivering nutrition; it’s also a way of establishing a relationship, requiring a sensitive dialogue between mother and infant… they learn to trust each other and to feel confident of each other’s love… This is baby’s first relationship in life and one that sets the tone for how baby learns to view the world.”
The Breastfeeding Book”, Martha Sears RN and William Sears, MD. Little Brown and Co., 2000.
It is so worth it. There is help available.
Types of courses
For Chiropractors and Bodyworkers

Learn to identify cranial, spinal, muscular and dural imbalances relating to breastfeeding as well as how to specifically address them. Gain current research to validate your work. Become familiar with the scope of other birth professionals in order to collaborate, gain referrals and provide the overall best care for your clients.
For Lactation Consultants and Birth Professionals

Learn specific infant anatomy in order to understand why your patient’s baby is struggling. Learn about the long term physical, emotional, and neurological implications of these issues. Become familiar with the scope of bodyworkers in order to provide the best support for your clients. Gain evidence based research to support your instincts.
For Breastfeeding
Parents

Gain resources to help you successfully breastfeed your baby without pain or struggle. Learn WHY breastfeeding is best. Why are you doing this? Understand how the alignment and
tone of your child’s body effects her development and long term health;
both neurologically and
emotionally.

