Not long ago, I was sitting around with some birthy friends of mine and, of course we were outside, properly socially distancing. Three of them are IBCLCs (lactation consultants) working in a hospital setting. The other one is a doula (birth coach). We all love to “talk shop” when we get together. The three IBCLCs were describing a new little patient they had seen recently. They used the term “failure to thrive”. This is a dreaded diagnosis for a newborn. They described this baby as not swallowing well and being overall “limp” in his body. Alarms were going off in my head and I thought to myself, “Oh My Gosh… I know exactly what is going on here”!
This leads to a very serious issue in the clinical breastfeeding world. John Hopkins Medical Center describes “Failure to Thrive” like this:
“Infants or children who fail to thrive have a height, weight and head circumference that do not match standard growth charts. The person’s weight falls lower than the third percentile (as outlined in standard growth charts) or 20 percent below the ideal weight for their height. Growing may have slowed or stopped after a previously established growth curve”.
Serious measures in the hospital and medical office are taken to make sure that the baby is transferring enough milk and gaining enough weight. If this is not happening, the baby will likely be put on formula to ensure rapid weight gain and begin testing for further complications. The matter is further complicated if the baby has an overall low Vagal tone. This basically means lowered parasympathetic function or, in layman’s terms- a reduction in heart/lung/digestion and other life sustaining functions which translates to a sort of limp and unresponsive baby. This combination of symptoms will set off alarms with the medical staff.
Soooo… Let’s address this dreaded diagnosis from the Cranial/Sacral standpoint knowing what we know about Cranial Nerves and the anatomy surrounding them. Failure to Thrive is often caused by…
TMJ (Temporal-mandibular) Dysfunction
The Temporal-mandibular joint (aka: the jaw) is a hinge joint made by the union of two cranial bones: the Temporals (on each side of the head) and the Mandible. These two bones are, in turn, connected to many other cranial bones. The mastoid processes of the Temporal bones sit in very close proximity to the atlas (C1) of the neck. Any misalignment of the cranial bones or the upper neck results in an imbalance of the TMJ. This also affects the normal alignment of the palate (the roof of the mouth). BABY CAN’T LATCH.
Weak muscles of the tongue
There are four extrinsic muscles that originate from the various cranial bones and the hyoid bone (located in the mid neck) which extend to the tongue; functioning to alter the tongue’s position which allows all of the ranges of motion needed for breastfeeding. Any misalignment or imbalance of these boney attachment sites pulls on the affected muscles, impeding their function.
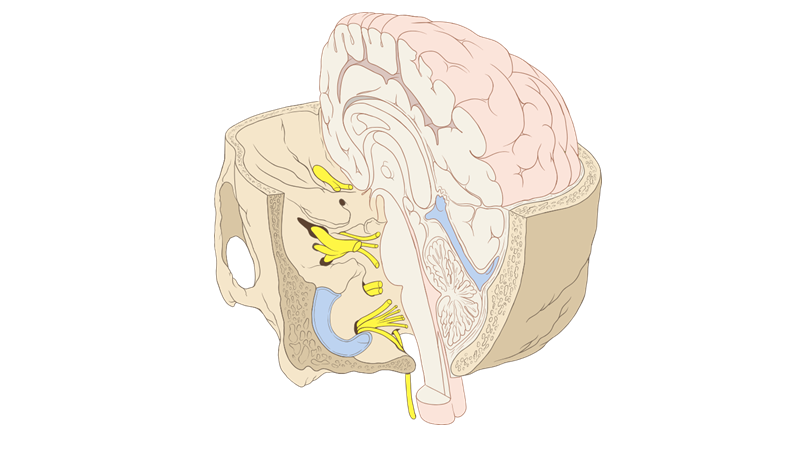
Cranial Nerve XII, the Hypoglossal Nerve, directly innervates the muscles of the tongue. This nerve exits the brain and exits from a small hole in the skull called the Hypoglossal Canal, which is located between the Upper cervical spine (the C1 vertebra) and Occiput. Any misalignment or imbalance at this area causes compression of this nerve and impedes its function. BABY CAN’T SUCK.
Weak Stylopharyngeaus Muscle
The Stylopharyngeaus Muscle forms the lateral walls of the pharynx. Its function is to elevate the larynx and the pharynx, and to dilate the pharynx (aka: swallowing).
It is directly innervated by Cranial Nerve IX, the Glossopharyngeal Nerve. This exits the brainstem through another small hole in the skull called the Vertebral Foramen, which is located between the Temporal bones (on the side of the cranium) and the Occiput (the base of the skull). In addition to the innervation, the Stylopharyngeus muscle stretches between the styloid process (of the Temporal bone) and the pharynx. Any misalignment or imbalance at this area causes compression of this CN IX and pulls on the muscle itself, impeding its function. BABY CAN’T SWALLOW.
Weak Vagus N (CN X)
The VAGUS nerve is the longest and most complex of the 12 pairs of cranial nerves that exit from the brain. It transmits information to/from the brain to tissues & organs elsewhere in the body. It functions as the main communication between the brain and the gut. It balances the heart rate and blood pressure. It allows for relaxation with deep breathing. It decreases inflammation. It plays a key role in fear management (anxiety). In essence, it controls all of the body’s life sustaining functions.
It exits the brainstem through that same little opening in the skull called the Vertebral Foramen, which is located between the Temporal bones (on the side of the cranium) and the Occiput (the base of the skull). Any misalignment or imbalance at this area causes compression of this nerve and impedes its function. BABY HAS A LOW VAGAL TONE.
John Hopkins Medical Center further describes some of the accepted causes for this condition:
- Complications of pregnancy and low birth weight
- Damage to the brain or central nervous system, which may cause feeding difficulties in an infant
- Heart or lung problems, which can affect how oxygen and nutrients move through the body
- Gastrointestinal problems that result in malabsorption or a lack of digestive enzymes
- Long-term gastroenteritis and gastroesophageal reflux (usually temporary)
Now, as we look at that list, we can correlate these causes with the cranial nerves and muscles involved AND how the structure and alignment of the body affects function. The gastrointestinal issues mentioned at the bottom of the list are associated with the nutritional advantages of breastmilk- i.e… breastmilk contains digestive enzymes while formula does not. We speak all about this in the Nutrition section of my course, “The Anatomy of Breastfeeding”.
Back to the opening story… My friends asked me what I thought about this baby’s condition and, of course, I was excited to give my very educated answer about all of these cranial nerve issues, but… unfortunately, bottom line… they replied that the WISHED that they could refer the baby to me.
Their hands were tied due to the restrictions of the hospital setting. There simply isn’t yet a continuity of practice within the Chiropractic profession, and especially among pediatric specialists to gain the confidence of the medical community. As I always say in my class… this is why it’s so important to train ourselves to do this work and to confidently educate other professionals about it. These babies need our help.

Here’s a great research article (abstract version) following one such case of FTT and the outcome after seeking Chiropractic care:
Resolution of Failure to Thrive in an Infant Following Chiropractic Care to Reduce Vertebral Subluxation: A Case Report & Review of the Literature
Jen Santos, DC, CACCP1 & Joel Alcantara, DC, PhDc2
Objective: To describe the positive health outcomes following chiropractic care in an infant diagnosed with failure to thrive.
Clinical Features: A-13-day-old male infant was presented by his parents for chiropractic consultation and possible care due to failure to thrive. According to the parents, he had lost a total of 27 ounces since birth. The parents were very distressed and tired due to having to provide around the clock care for their newborn to keep him alive. He was inconsolable most of the time. Breastfeeding was difficult.
His mother described him as lethargic with a very weak cry. Medical intervention did not help. Intervention and Outcome: The infant was cared for with a sustained contact “touch and hold” spinal adjustment to sites of subluxations at the cervico-cranio-mandibular complex. After eight visits within two weeks, the breastfeeding difficulty had resolved as his weight increased from 5 lbs. 1oz. to 6 lbs. 12oz.
Conclusion: This case report highlights the benefits of chiropractic in infants suffering from failure to thrive. Given the benefits of chiropractic care for their child as described above, his parents chose to continue wellness chiropractic care for him. The infant is assessed for vertebral subluxation and adjusted accordingly approximately 2-3 times a month. As a long-term follow-up, at 2.5 years of old, his height and weight were within normal limits for his age and his neurological and motor skills were intact and within normal limits.
Let’s look at this issue on a global front. According to the WHO (World Health Organization)…
Over 820,000 children’s lives could be saved every year among children under 5 years, if all children 0–23 months were optimally breastfed. They define “optimally breastfed” to mean the initiation of breastfeeding within 1 hour of birth, exclusive breastfeeding for the first 6 months of life, and the Introduction of nutritionally-adequate and safe complementary (solid) foods at 6 months with continued breastfeeding up to 2 years old.
Breastfeeding is one of the most effective ways to ensure child health and survival. Undernutrition is associated with 45% of child deaths (2.7 million child deaths annually). The first 2 years of a child’s life are particularly important, as optimal nutrition during this period lowers morbidity and mortality, reduces the risk of chronic disease, and fosters better development overall.
Gentle adjustments and cranial therapy can not only improve breastfeeding, but it can actually be life-saving.
To learn more about breastfeeding and the anatomy involved in infants and how it affects breastfeeding, real-life case studies with breastfeeding patients, a host of interviews with lactation consultants, diagrams, demonstrations, and visual examples to teach the global subluxation pattern – The Anatomy of Breastfeeding. This new, updated, accredited continuing education course is for Chiropractors who are looking to improve their careers, learn from leaders and experts in their industry, and looking for new opportunities! The course is approved for 10 chiropractic CE hours.

